Cranial nerves (sometimes termed
cerebral nerves),
[1] are
nerves that emerge directly from the
brain and the
brainstem, in contrast to
spinal nerves (which emerge from various segments of the
spinal cord). Information is exchanged between the brain and various regions, primarily of the head and neck, via the cranial nerves.
[2]
Spinal nerves reach as far as the first cervical vertebra, and the cranial nerves fill a corresponding role above this level.
[3]
Each cranial nerve is paired and is present on both sides. Depending on
source there are in humans twelve or thirteen pairs of cranial nerves,
which are assigned
Roman numerals I-XII,
[2] and zero assigned to
cranial nerve zero,
[4] according to the order in which they originate from the forebrain to the back of the brain and the brainstem.
[2]
Cranial nerves 0, I and II emerge from the
cerebrum or forebrain;
[5] the remaining ten pairs emerge from the brainstem.
The cranial nerves are components of the
peripheral nervous system (PNS), with the exception of cranial nerve II (the
optic nerve), which is not a true
peripheral nerve but a
neural tract of the
diencephalon connecting the
retina with the
lateral geniculate nucleus; hence both the optic nerve and the retina are part of the
central nervous system (CNS).
[6] The
axons of the remaining twelve nerves extend beyond the brain and are considered part of the PNS.
[7] The central
ganglia of the cranial nerves or
cranial nerve nuclei originate in the CNS, preferentially from the
brainstem.
Anatomy
Terminology
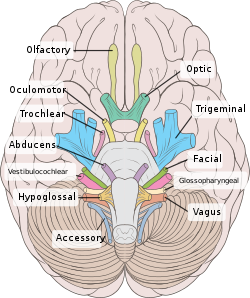
Inferior schematic view of the
brain and
brainstem showing the
cranial nerves, numbered from olfactory to hypoglossal after the order in which they emerge.

Inferior view of the human brain showing the cranial nerves as visible on an autopsy specimen.
Traditionally, among humans there are considered to be twelve cranial
nerves, numbered I-XII, all of which are paired. The cranial nerves
arise directly from the central nervous system; the first two pairs, I
and II, arise from the base of the
forebrain, and the others, nerves III to XII, arise from the
brainstem. Their naming scheme is given after their
rostral-caudal orientation,
[3][8] as, when viewing the brain and brainstem from below, they are often visible in their numeric order.
Unique
anatomical terminology is used to describe the course of the cranial nerves. Like all nerves, the nerves have a
nucleus, and a course within and outside of the brain. The course within the brain is known as the
central course of the nerve, and the course after it has emerged from the brain as the
peripheral course. The nerves are
paired,
which means that they occur on both the right and left sides. Some
nerves cross from the right side to the left side, and this is known
anatomically as
decussating. If a nerve supplies a muscle, skin,
or has another function on the same side of the body as where it
originates, this is called an
ipsilateral course. If the course is opposite to the nucleus of the nerve, this is known as a
contralateral course.
Intercranial course
The cranial nerves serve to innervate the head and neck area,
[8] including both
somatic and
autonomic motor innervation as well as sensory innervation. Together the cranial nerves supply sensory innervation of the
special senses such as
taste,
vision;
smell;
hearing. They also supply afferens of the
somatic senses:
visceral sensation of the head and neck;
balance, and
proprioception combining
vestibular perception with proprioceptive information from the head and neck.
[9]
Distinct from the head the two cranial nerves: IX and X; the
glossopharyngeal and vagus nerves innervate both motor and sensory
synapses pertaining to
abdominal organs (though not
pelvic), as well as structures of the
neck and
chest.
[3]
Differentiating the cranial nerves from spinal nerves, the cranial
nerves are not strictly bound to certain segments of the body (as in
dermatomes), but rather organize after function, hence the innervated areas overlap significantly more than those of spinal nerves.
[3] The
accessory nerve XI, is considered either a cranial nerve or a spinal nerve which emanates level with the brain-stem.
[3]
Similar to the
dorsal root ganglia of the
spinal nerves and parasympathetic ganglia of the
sacral parasympathetic system, the sensory cranial nerves have a number of
ganglia outside the central nervous system. The sensory ganglia are directly correspondent to dorsal root ganglia and are as known as
cranial sensory ganglia, and found along the course of the cranial nerves, outside the brain
[8] and skull. Sensory ganglia exist for nerves with sensory function; V, VII, VIII, IX, X.
[3] There are also a number of
parasympathetic cranial nerve ganglia, while
sympathetic ganglia innervating the head and neck reside in the upper regions of the
sympathetic trunk, and do not belong to the cranial nerves.
[10]
Nuclei

The brainstem, with brainstem
cranial nerve nuclei and tracts inside the brainstem shaded red to illustrate the deeper structures.
The nerve fibres in each nerve contain a nucleus either in the brainstem of the
mesencephalon. The
olfactory nerve (I) emerges from the
olfactory bulb, and depending slightly on division the
optic nerve (III) is deemed to emerge from the
lateral geniculate nuclei. The rest of the nerves have their cell-bodies in the brainstem and thus originate in the brainstem.
[10]
Cranial nerve columns
Brainstem showing motor nuclei in red, and sensory nuclei in blue.
Brainstem nuclei with associated functions are often found in similar
areas of the brainstem. These are also known as functional columns.
[10] Functional columns are a result of the development of the spinal cord. Four columns of
gray matter are present in the spinal cord during embryological development. Each column represents a different function, and contributes
neurons to different nerves. Each nerve is innervated by neurons from one or more of the columns.
[9]
As the spinal cord develops, there are four columns. These are the
general somatic efferent column, the general visceral efferent column,
the general visceral afferent column and general somatic afferent
column. These columns also extend into the brainstem, but are divided
into smaller pieces.
[9] In the brainstem there are six columns.
Four 'general' columns contain fibres that supply sensation or control muscles:
[11]
There are three additional columns which innervate organs and tissues developing from the
branchial arches and
inner ear. These are the following:
With the exception of the olfactory nerve (I) and optic nerve (II), the cranial nerves emerge from the
brainstem. The oculomotor nerve (III) and trochlear nerve (IV) emerge from the
pons, the trigeminal (V), abducens (VI), facial (VII) and vestibulocochlea (VIII) from the
midbrain, and the glossopharyngeal (IX), vagus (X), accessory (XI) and hypoglossal (XII) emerge from the
medulla.
[12]
The olfactory nerve (I) and optic nerve (II) emerge separately. The olfactory nerves emerge from the
olfactory bulbs on either side of the
crista galli, a bony projection below the
frontal lobe, and the optic nerves (II) emerge from the
lateral colliculus, swellings on either side of the
temporal lobes of the brain.
[12]
Exiting the skull
After emerging from the brainstem, the cranial nerves travel through the
skull,
but must leave this bony compartment in order to reach their
destinations. Some nerves pass through unique holes in the skull, called
foramina,
as they travel to their destination. Other nerves pass through bony
canals, longer canals enclosed by bone. These foramina and canals may
contain more than one cranial nerve, and may also contain additional
blood vessels.
[11]
- The olfactory nerve (I) passes through the cribiform plate, many small perforations in the ethmoid plate.
- The optic nerve (II) passes through the optic foramen as it travels to the eye.
- The oculomotor nerve (III), trochlear nerve (IV), abducens nerve
(VI) and the opthalamic branch of the trigeminal nerve (V1) travel
through the cavernous sinus into the superior orbital fissure, passing out of the skull into the orbit.
- The maxillary division of the trigeminal nerve (V2) passes through the round foramen
- The mandibular division of the trigeminal nerve (V3) passes through the oval foramen
- The facial nerve (VII) and vestibulocochlear nerve (VIII) both pass through the internal auditory canal
The cranial nerves commonly enter and exit the skull together, for
example nerves II, III, IV, V, and VI all pass through foramina near the
pituitary fossa.
[3]
The facial nerve enters the temporal bone at the internal acoustic
meatus but exits the skull via the stylomastoid foramen while the
vestibulocochlear nerve never actually exits the skull.
Ganglia
The cranial nerves give rise to a number of
ganglia, collections of the
cell bodies of neurons in the nerves that are outside of the brain. These ganglia are both parasympathetic and sensory ganglia.
The ganglion of the sensory nerves, which are similar in structure to the
dorsal root ganglion of the
spinal cord, include:
[13]
Additional ganglia for nerves with
parasympathetic function exist, and include the
Ciliary ganglion of the oculomotor nerve (III), the
pterygopalatine ganglion of the maxillary nerve (V2), the
submandibular ganglion of the
lingual nerve, a branch of the facial nerve (VII), and the
otic ganglion of the glossopharyngeal nerve (IX).
[14]
Course
The following images show the cranial nerves schematically showing
their respective exits from the CNS or brain-stem (not including the
optic nerve which does not leave the CNS), and their path, as well as
conceptual innervation targets.
-
-
-
-
3 The
oculomotor controls a number of motor function of the eye, both somatic and autonomic.
-
-
5 The
trigeminal innervates a large number of structures, both motor and sensory.
-
-
7 The
facial nerve stands for innervation of a large number of structures both motor and sensory.
-
-
9 The
glossopharyngeal innervates a number of motor and sensory structures of the tongue and pharynx.
-
10 The
vagus nerve innervates a large number of
parasympathetic synapses of the head, neck, thorax and upper abdomen. It also has motor innervation to the trachea, larynx and bronchi.
-
-
Summary
| No. |
Name |
Sensory,
motor,
or both |
Origin/Target |
Function |
| 0 |
Terminal |
Purely sensory |
Lamina terminalis |
Animal research indicates that the terminal nerve is involved in the detection of pheromones.[15][unreliable medical source?][16] |
| I |
Olfactory |
Purely sensory |
Telencephalon |
Transmits the sense of smell from the nasal cavity.[17] Located in the olfactory foramina in the cribriform plate of the ethmoid bone. |
| II |
Optic |
Sensory |
Retinal ganglion cells |
Transmits visual signals from the retina of the eye to the brain.[18] Located in the optic canal. |
| III |
Oculomotor |
Mainly motor |
Anterior aspect of Midbrain |
Innervates the levator palpebrae superioris, superior rectus, medial rectus, inferior rectus, and inferior oblique, which collectively perform most eye movements. Also innervates the sphincter pupillae and the muscles of the ciliary body. Located in the superior orbital fissure. |
| IV |
Trochlear |
motor |
Dorsal aspect of Midbrain |
Innervates the superior oblique muscle, which depresses, rotates laterally, and intorts the eyeball. Located in the superior orbital fissure. |
| V |
Trigeminal |
Both sensory and motor |
Pons |
Receives sensation from the face and innervates the muscles of mastication.
- Located in the;
-
- superior orbital fissure (ophthalmic nerve - V1),
- foramen rotundum (maxillary nerve - V2),
- foramen ovale (mandibular nerve - V3).
|
| VI |
Abducens |
Mainly motor |
Nuclei lying under the floor of the fourth ventricle
Pons |
Innervates the lateral rectus, which abducts the eye. Located in the superior orbital fissure. |
| VII |
Facial |
Both sensory and motor |
Pons (cerebellopontine angle) above olive |
Provides motor innervation to the muscles of facial expression, posterior belly of the digastric muscle, stylohyoid muscle, and stapedius muscle. Also receives the special sense of taste from the anterior 2/3 of the tongue and provides secretomotorinnervation to the salivary glands (except parotid) and the lacrimal gland. Located in and runs through the internal acoustic canal to the facial canal and exits at the stylomastoid foramen. |
| VIII |
Vestibulocochlear
(also auditory,[19] acoustic,[19] or auditory-vestibular) |
Mostly sensory |
Lateral to CN VII (cerebellopontine angle) |
Mediates sensation of sound, rotation, and gravity (essential for
balance and movement). More specifically, the vestibular branch carries
impulses for equilibrium and the cochlear branch carries impulses for
hearing. Located in the internal acoustic canal. |
| IX |
Glossopharyngeal |
Both sensory and motor |
Medulla |
Receives taste from the posterior 1/3 of the tongue, provides secretomotor innervation to the parotid gland, and provides motor innervation to the stylopharyngeus. Some sensation is also relayed to the brain from the palatine tonsils. Located in the jugular foramen. This nerve is involved together with the vagus nerve in the gag reflex. |
| X |
Vagus |
Both sensory and motor |
Posterolateral sulcus of Medulla |
Supplies branchiomotorinnervation to most laryngeal and pharyngeal muscles (except the stylopharyngeus, which is innervated by the glossopharyngeal). Also provides parasympathetic fibers to nearly all thoracic and abdominal viscera down to the splenic flexure.
Receives the special sense of taste from the epiglottis. A major
function: controls muscles for voice and resonance and the soft palate.
Symptoms of damage:dysphagia (swallowing problems), velopharyngeal insufficiency. Located in the jugular foramen. This nerve is involved (together with nerve IX) in the pharyngeal reflex or gag reflex. |
| XI |
Accessory
Sometimes:
cranial accessory
spinal accessory |
Mainly motor |
Cranial and Spinal Roots |
Controls the sternocleidomastoid and trapezius muscles, and overlaps
with functions of the vagus nerve (CN X). Symptoms of damage: inability
to shrug, weak head movement. Located in the jugular foramen. |
| XII |
Hypoglossal |
Mainly motor |
Medulla |
Provides motor innervation to the muscles of the tongue (except for the palatoglossal muscle, which is innervated by the vagus nerve) and other glossal muscles. Important for swallowing (bolus formation) and speech articulation. Passes through the hypoglossal canal. |
Function
Cranial nerve function is an important element in
neurological examination,
as specific dysfunction may indicate as to which portion of the
brainstem is damaged. It is of clinical importance to know the path and
origin of the cranial nerves, both intracranially as well as
extracranially.
[3]
The cranial nerves are often the first structures to be affected by different forms of
brain injury such as
hemorrhaging or
tumors, partly because they are sensitive to compression.
[10] Mononeuropathy of a cranial nerve may sometimes be the first symptom of an
intracranial or
skull base cancer.
[20]
Smell (I)
Damage to the olfactory nerve can cause an inability to smell (
anosmia), a distortion in the sense of smell (
parosmia),
or a distortion or lack of taste. Specific testing is performed when an
individual perceives lack of taste or affected taste. The smell from
each nostril is tested individually, and with consideration of airflow.
Different substances are used, and these include coffee or soap. Using
stronger smelling substances, for example ammonia, may lead to the
activation of nociceptors of the trigeminal nerve.
[21]
Vision (II)
Damage to the optic nerve affects vision. Vision is affected
depending on the location of the lesion. A person may not be able to see
things on their left or right side (
homonymous hemianopsia), or may have difficulty seeing things on their outer visual fields (
bitemporal hemianopsia) if the
optic chiasm is involved.
[1]:82 Vision may be tested using a number of different tests, examining the
visual field, or by examining the cornea with a
ophthalmoscope, using a process known as
funduscopy. Visual field testing may be used to pin-point structural lesions in optic nerve, or further along the visual pathways.
[21]
Eye movement (III, IV, VI)

Various deviations of the eyes due to abnormal function of the targets of the cranial nerves
Damage or lesion of nerves III, IV, or VI may affect the movement of
the eye or pupil. Either both or one eye may be affected, and if both
eyes are affected no double vision (
diplopia)
will occur. These nerves might be examined by observing how the eye
follows an object in different directions. This object may be a finger
or a pin, and may be moved at different directions to test for
pursuit velocity.
[21]
If the eyes do not work together, the most likely cause is damage to a specific cranial nerve or nuclei.
[21]
-
- Damage to the oculomotor nerve can cause double vision (diplopia) with lateral strabismus, and also ptosis and mydriasis.[1]:84 All but specific deviations may be due to damage in this nerve or any of the muscles it innervated, (though not internuclear ophthalmoplegia). Lesion may also lead to inability to open the eye, due to disrupted innervation of the levator palpebrae (unlike in Horner syndrome,
which only results in a droopy eyelid. Individuals suffering from
lesion or damage to the oculomotor nerve may compensate by tilting their
heads to alleviate symptoms due to lack of control from oblique muscles when the eye is not adducted.[21]
- Damage to the trochlear nerve can also cause diplopia with the eye adducted and elevated.[1]:84
The result will be an eye which can not move downwards or inwards
properly (especially downwards when in an inward position). This is due
to impairment in the superior oblique muscle innervated by the trochlear nerve.[21]
- Damage to the abducens nerve can also result in diplopia with medial strabismus.[1]:84 This is due to impairment in the lateral rectus muscle innervated by the nerve.[21]
Facial sensation (V)
Conditions affecting the trigeminal nerve include
trigeminal neuralgia,
[10] cluster headache,
[22] and trigeminal
zoster.
[10] Trigeminal neuraliga occurs later in life, from
middle age
onwards, most often after an age of 60; and is a condition associated
with very strong pain distributed over the area innervated by the
trigeminal nerve. Often the pain follows the distribution of the
maxillary or
mandibular nerve, (branches V
2 and V
3.
[23] The trigeminal nerve is also present in the
tendon reflexive jaw jerk. A
reflex
involving an induced twitch in muscles involved in closing the jaw when
upon tapping on the jaw. A stronger reflex may be present if there is a
supranuclear lesion of the trigeminal nerves motor nucleus, for example
in
pseudobulbar palsy.
[23] In
Parkinson's disease the trigeminal nerve is involved in the
glabellar reflex which causes involuntary eye-blinking.
Facial expression (VII)
Lesions of the facial nerve may manifest as
facial palsy.
This is where a person is unable to move the muscles on one or both
sites of their face. If only the peripheral nerve itself is affected,
this may cause
Bell's palsy.
Palsy that occurs is on the same side of the affected nerve. Central
facial palsy will manifest in a similar fashion. If the nerve is damaged
only on one side, a person will still be able to raise the eyebrows and
crease the forehead on that side. That is because the
frontalis muscle
is innervated by both the left and the right cranial nerve. The effect
is most often unilateral, and indicates contralateral damage or
engagement of the cerebrum.
[10]
Hearing and balance (VIII)
The vestibulocochlear nerve splits into the
vestibular and
cochlear nerve. The vestibular part is responsible for innervating the
vestibules and
semicircular canal of the
inner ear, which transmits information about
balance, and is an important component of the
vestibuloocular reflex, which keeps the head stable and allows the eyes to track moving objects. The
cochlear nerve transmits information from the
cochlea, allowing sound to be heard.
When damaged:
- The vestibular nerve may give rise to the sensation of spinning and dizziness, and may cause rotatory nystagmus. Function of the vestibular nerve may be tested through caloric stimulation.[21] Damage to the vestibulocochlear nerve can also present as repetitive and involuntary eye movements (nystagmus), particularly when looking in a horizontal plane.[21]
- The cochlear nerve will cause partial or complete deafness in the affected ear.[21]
Oral sensation and taste (IX)

Deviating uvula due to cranial nerve X lesion.
The glossopharyngeal nerve is almost exclusively sensory in supplying
five afferent nuclei of the brainstem, covering the oropharynx and back
of the tongue with innervation.
[24] Damage may result in difficulties swallowing.
[21]
Vagus nerve (X)
Loss of function of the vagal nerve will lead to a loss of
parasympathetic innervation to a very large number of structures. Of the
major effects a rise in blood pressure and heart rate may occur.
Isolated dysfunction of only the vagus nerve is rare, but can be
diagnosed by a hoarse voice, due to dysfunction of the
superior laryngeal nerve[10]
Testing of function may be performed by assessing ability to drink
liquids. Choking on either saliva or liquids may indicated neurological
damage to the vagal nerve.
[21] Damage to the glossopharyngeal can be assessed by asking the subject to say "Ah" during phonation inspect to see if the
uvula
deviates. Positive sign indicative of unilateral damage occurs with
finding of asymmetrically deviating uvula, towards the side with an
intact or healthy nerve.
[21]
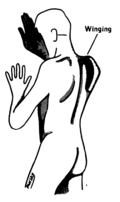
Shoulder elevation and head-turning (XI)
Damage to the accessory nerve may lead to contralateral weakness in the
trapezius, which can be tested by asking the subject to raise their shoulders or shrug, upon which the
scapula will move out into a
winged position if the nerve is damaged.
[21] Weakness or an inability to elevate the scapula may be present, since the
levator scapulae is alone in providing this function.
[23]
There may also be weakness present of the
sternocleidomastoid muscle, but as it received cortical innervation from the ipilateral side any damage will give rise to ipsilateral weakness.
[21]
Tongue movement (XII)

A damaged hypoglossal nerve will result in an inability to stick the tongue out straight.
The hypoglossal nerve is unique in that it is innervated bilaterally
from both hemispheres motor cortex. Damage to the nerve at lower motor
neuron level may lead to fascinations of atrophy of the musculature of
the tongue. The fasciculations of the tongue are sometimes said to look
like a "bag of worms". Upper motor neuron damage will not lead to
atrophy or fasciculations, but only weakness of the innervated muscles.
[21]
When the nerve is damaged it will lead to unilateral weakness, and
the tongue will upon being stuck out move towards the weaker or damaged
side, as shown in the image.
[21]
Clinical significance
Exam
Doctors,
neurologists and other medical professionals may conduct a
cranial nerve examination as part of a
neurological examination to examine the cranial nerves. This is a highly formalised series of steps involving specific tests for each nerve.
Damage
Stroke
Stroke
may damage the blood supply to areas of the nerves. It may also damage
the areas of the brain that control the nerves. If there is a stroke of
the
midbrain,
pons or
medulla, various cranial nerves may be damaged, resulting in dysfunction and symptoms of
a number of different syndromes.
Cavernous sinus thrombosis refers to a
thrombus affecting the venous drainage from the
cavernous sinus, which several cranial nerves pass through.
Compression
Nerves may be compressed because of increased
intercranial pressure or tumour masses that presses against the nerves. For example, an
optic glioma may impact on the optic nerve (II), and an
acoustic neuroma may compress the facial nerve (VII) and vestibulocochlear nerve (VIII)
Inflammation
Inflammation can be a result of infection, such as viral causes, or
can occur spontaneously. Inflammation is more common in some nerves than
others. Spontaneous inflammation may result in a palsy of a nerve that
self-resolves, such as
Trochlea palsy. Inflammation of the facial nerve (VII) may result in
Bell's palsy. Inflammation of the trigeminal nerve (V) may result in
Trigeminal neuralgia, a phenominon in which the face is exquisitely tender.